Dr. Elizabeth Vance, PsyD, LCSW
🛡️ Verified ClinicianLicensed Clinical Psychologist & Psychotherapist
Dr. Vance is a licensed clinical psychologist and somatic therapy pioneer with over 14 years of clinical outpatient experience. She specializes in cognitive behavioral therapy (CBT), somatic down-regulation techniques, and values-based emotional regulation frameworks.
PTSD treatment is no longer a one-size-fits-all approach. Modern trauma-informed care has evolved dramatically over the past two decades, offering survivors of traumatic experiences a diverse, evidence-based toolkit for genuine healing and lasting recovery.
Whether your trauma stems from combat exposure, childhood abuse, sexual assault, a serious accident, or prolonged emotional neglect, effective PTSD treatment exists that can help you reduce symptoms, rebuild your nervous system’s sense of safety, and reclaim a meaningful, connected life.
In this comprehensive guide, we explore the most clinically validated treatment modalities, emerging therapeutic approaches, and practical strategies that make real recovery possible.

Understanding PTSD Before Exploring Treatment
Post-traumatic stress disorder (PTSD) is a complex neurobiological condition that develops when the brain and nervous system become stuck in a chronic state of threat activation following traumatic experiences. It is not a sign of weakness, a character flaw, or an inability to cope. It is a predictable physiological response to overwhelming experiences that exceeded your nervous system’s capacity to process at the time they occurred.
PTSD affects approximately 20 million adults in the United States at any given time, cutting across every demographic, age group, profession, and background. Combat veterans, first responders, survivors of domestic violence, childhood trauma survivors, and individuals who have experienced sudden loss or life-threatening illness all face significant PTSD risk.
This YouTube video above explains post-traumatic stress disorder (PTSD), highlighting symptoms, causes, and treatment options. It shows how PTSD affects mental health. Understanding this helps recognize and manage the condition.
Core PTSD Symptom Clusters
Accurate understanding of PTSD’s symptom profile is foundational to selecting the most appropriate PTSD treatment approach. The DSM-5 identifies four primary symptom clusters:
- Intrusion symptoms: Flashbacks, intrusive memories, nightmares, and intense psychological distress when exposed to trauma reminders
- Avoidance symptoms: Deliberate avoidance of trauma-related thoughts, memories, people, places, or activities
- Negative alterations in cognition and mood: Persistent shame, guilt, distorted self-blame, emotional numbness, feeling detached from others, loss of interest in previously enjoyed activities
- Hyperarousal and reactivity: Hypervigilance, exaggerated startle response, irritability, angry outbursts, reckless behavior, and significant sleep disturbances
These symptom clusters interact and compound one another, creating a self-reinforcing cycle that makes recovery feel impossible without proper support and structured PTSD treatment.
Why Specialized PTSD Treatment Matters
General talk therapy, while valuable for many mental health concerns, is insufficient for treating PTSD effectively. Trauma memories are stored differently from ordinary memories. They are encoded in a fragmented, sensory-dominated format that is not easily accessible through conventional verbal processing alone.
Effective PTSD treatment must address the whole person, including the body’s physiological trauma responses, the nervous system’s dysregulation, the cognitive distortions that trauma creates, and the relational wounds that often accompany traumatic experiences. This is why trauma-specialized approaches consistently outperform general counseling in clinical outcome research.
8 Proven PTSD Treatment Approaches
1. Trauma-Focused Cognitive Behavioral Therapy (TF-CBT)
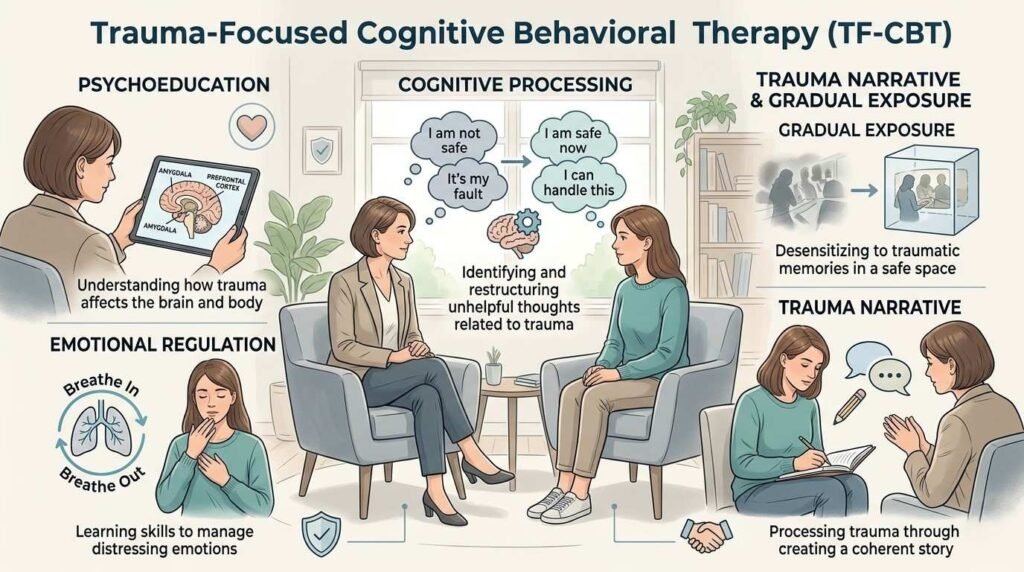
Trauma-focused cognitive behavioral therapy is one of the most extensively researched and clinically validated PTSD treatment modalities available. TF-CBT directly addresses the distorted thought patterns, avoidance behaviors, and emotional responses that maintain PTSD symptoms long after the traumatic event has ended.
Core components of TF-CBT include:
- Psychoeducation about trauma and PTSD symptoms
- Relaxation and emotional regulation skills development
- Cognitive processing of trauma-related beliefs and meanings
- Gradual exposure to trauma memories in a safe, controlled therapeutic context
- Trauma narrative development to process and integrate fragmented memories
Research consistently demonstrates that TF-CBT produces significant symptom reduction in 70 to 90 percent of participants who complete a full treatment course, making it a cornerstone of evidence-based PTSD treatment.
2. EMDR Therapy (Eye Movement Desensitization and Reprocessing)

EMDR therapy represents one of the most significant breakthroughs in PTSD treatment in recent history. Developed by Dr. Francine Shapiro in the late 1980s, EMDR uses bilateral sensory stimulation, typically guided eye movements, alternating taps, or auditory tones, to help the brain reprocess stuck traumatic memories.
The core principle behind EMDR is that traumatic memories become frozen in their original, overwhelming form because the brain’s natural memory processing system was overwhelmed at the time of the trauma. Bilateral stimulation during EMDR activates this dormant processing system, allowing traumatic memories to be reprocessed into a less distressing, more integrated narrative form.
EMDR is endorsed as a first-line PTSD treatment by:
- World Health Organization (WHO)
- American Psychiatric Association (APA)
- Department of Veterans Affairs (VA)
- International Society for Traumatic Stress Studies (ISTSS)
Clinical trials demonstrate that EMDR produces significant PTSD symptom reduction in as few as 6 to 12 sessions, with many patients experiencing complete symptom remission.
3. Prolonged Exposure Therapy (PE)

Prolonged exposure therapy is a structured, evidence-based PTSD treatment approach developed by Dr. Edna Foa at the University of Pennsylvania. PE is grounded in the understanding that trauma recovery requires carefully guided engagement with avoided memories, feelings, and situations rather than continued avoidance.
PE typically involves two core components:
- In vivo exposure: Gradually approaching safe situations, places, and activities that have been avoided because of their association with the trauma
- Imaginal exposure: Revisiting the traumatic memory in detail within the safety of the therapeutic relationship, allowing emotional processing and meaning-making to occur
Research consistently shows that prolonged exposure reduces PTSD symptoms significantly and maintains treatment gains at long-term follow-up, making it one of the most durable PTSD treatment options available.
4. Cognitive Processing Therapy (CPT)
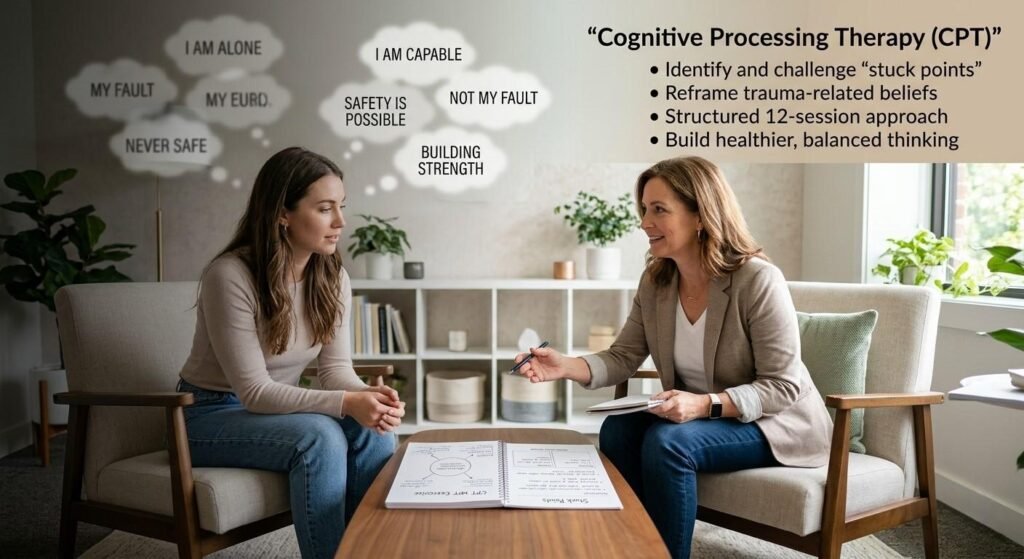
Cognitive processing therapy is a highly structured PTSD treatment that focuses specifically on identifying and challenging the unhelpful beliefs that trauma creates about oneself, others, and the world. These are called stuck points, and they perpetuate PTSD by maintaining a worldview distorted by traumatic experience.
Common stuck points that CPT addresses include beliefs such as:
- “It was my fault that this happened to me”
- “I should have done something to prevent it”
- “The world is completely dangerous”
- “I am permanently damaged and broken”
- “No one can be trusted”
CPT is delivered over 12 structured sessions and has strong evidence of effectiveness across diverse trauma populations, including combat veterans, sexual assault survivors, and childhood trauma survivors. It is one of the VA’s most recommended PTSD treatment approaches for military personnel.
5. Somatic Experiencing and Body-Based PTSD Treatment

Conventional talk-based therapies alone often fail to address the body-held dimensions of traumatic stress. Trauma researcher Dr. Bessel van der Kolk’s landmark work, encapsulated in his seminal book “The Body Keeps the Score,” demonstrates that PTSD is fundamentally a dysregulation of the body’s physiological threat response system.
Somatic Experiencing (SE), developed by Dr. Peter Levine, approaches PTSD treatment through the body’s own natural capacity for trauma resolution. SE works by:
- Tracking bodily sensations associated with traumatic activation
- Titrating exposure to trauma material in very small, manageable doses
- Completing interrupted defensive responses that were frozen at the moment of trauma
- Restoring the nervous system’s natural rhythm between activation and relaxation
Other body-based PTSD treatment modalities include Sensorimotor Psychotherapy, yoga-based trauma therapies, and neurofeedback, all of which address the physiological dimension of trauma that talk therapy alone cannot fully reach.
6. Internal Family Systems Therapy (IFS)
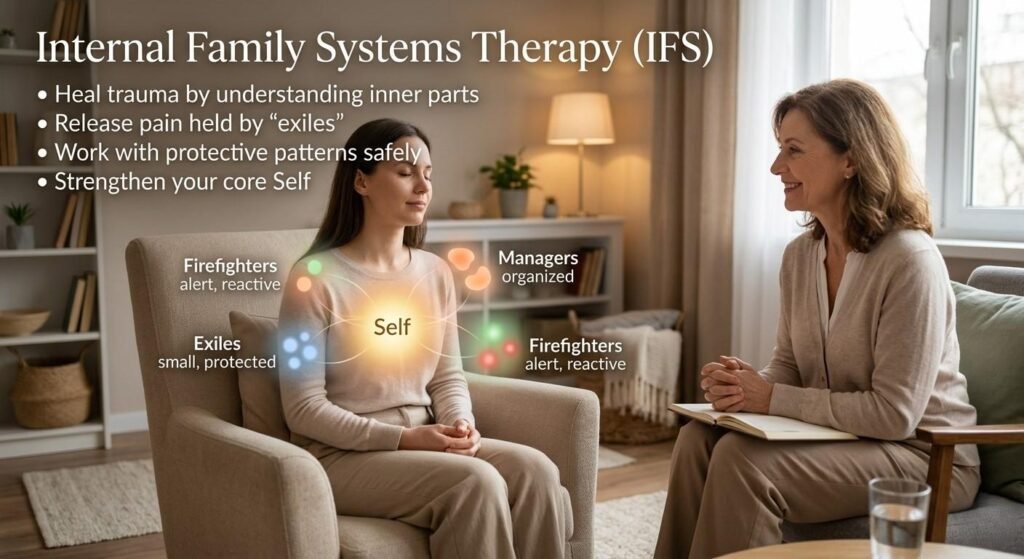
Internal Family Systems therapy, developed by Dr. Richard Schwartz, has emerged as a profoundly effective PTSD treatment approach, particularly for complex trauma and childhood trauma survivors. IFS operates on the understanding that the mind is naturally composed of multiple parts, each with its own perspective, protective role, and emotional history.
In the context of PTSD treatment, IFS identifies:
- Exiles: Vulnerable parts carrying the pain, shame, and fear of traumatic experiences
- Managers: Protective parts that work hard to keep the person functional and prevent exile pain from surfacing
- Firefighters: Reactive parts that engage in impulsive or self-destructive behaviors to suppress overwhelming emotional flooding
IFS PTSD treatment involves building a trusting relationship with each protective part, gently accessing and healing exiled parts carrying trauma burdens, and strengthening the Self, the calm, compassionate core of the person that has never been damaged by trauma.
7. Medication-Based PTSD Treatment
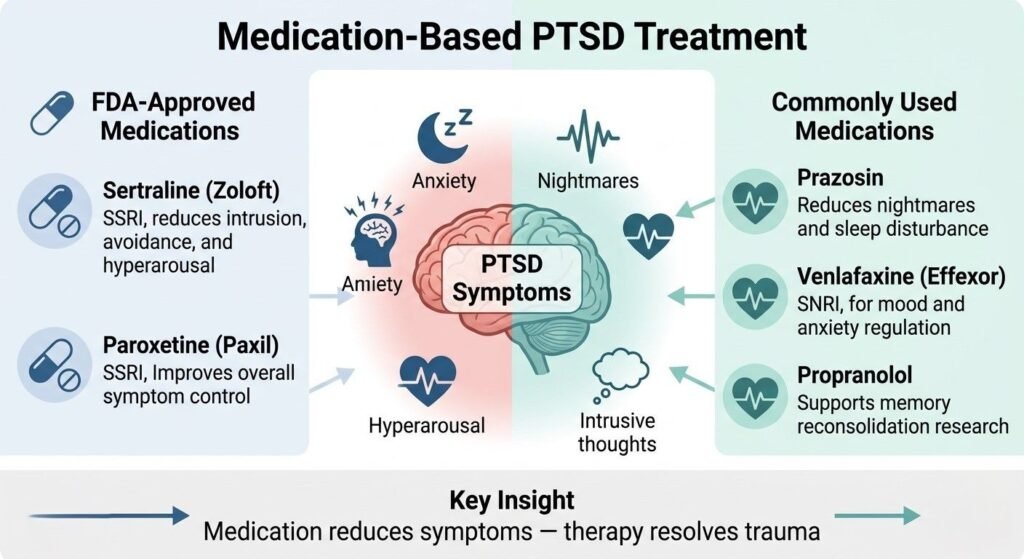
While therapy forms the foundation of effective PTSD treatment, medication can play an important supportive role, particularly in reducing the severity of symptoms that make engaging in trauma-focused therapy difficult.
Currently, the FDA has approved two medications specifically for PTSD treatment:
- Sertraline (Zoloft): An SSRI antidepressant shown to reduce intrusion, avoidance, and hyperarousal symptoms
- Paroxetine (Paxil): Another SSRI with demonstrated effectiveness for PTSD symptom management
Additional medications frequently used in PTSD treatment include:
- Prazosin: An alpha-blocker particularly effective for PTSD-related nightmares and sleep disturbances
- Venlafaxine (Effexor): An SNRI with growing evidence for PTSD symptom reduction
- Propranolol: Being researched for its potential to reduce traumatic memory reconsolidation
It is important to understand that medication addresses PTSD symptoms rather than resolving the underlying traumatic memories. Optimal outcomes typically result from combining medication with trauma-focused psychotherapy.
8. MDMA-Assisted Psychotherapy for PTSD
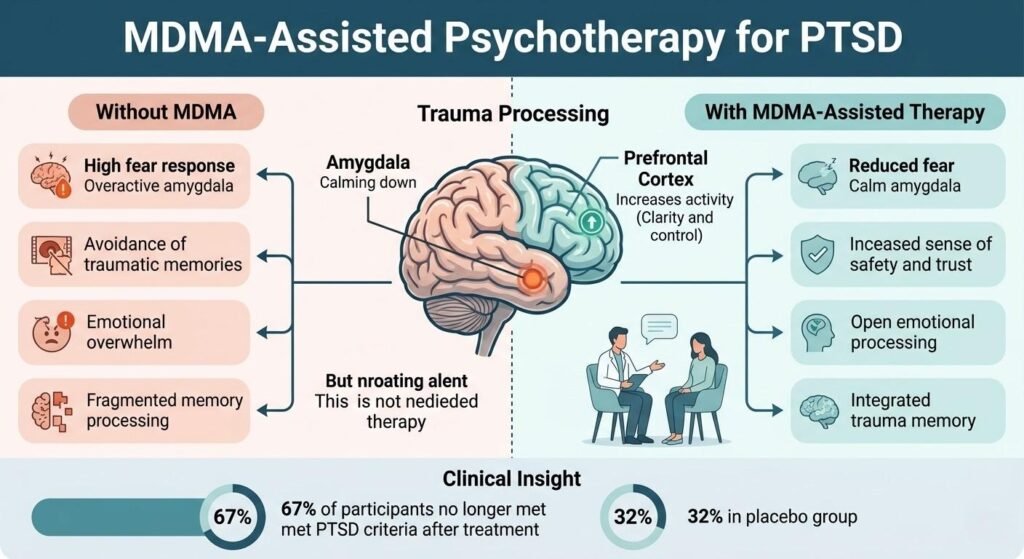
Among the most exciting developments in PTSD treatment research is MDMA-assisted psychotherapy. Phase 3 clinical trials conducted by the Multidisciplinary Association for Psychedelic Studies (MAPS) demonstrated that MDMA-assisted therapy produced 67 percent of participants no longer meeting PTSD diagnostic criteria after treatment, compared to 32 percent in the placebo group.
MDMA-assisted PTSD treatment works by temporarily reducing amygdala reactivity and fear response while increasing feelings of safety, empathy, and openness, creating an optimal neurobiological state for processing traumatic memories that would otherwise be too overwhelming to approach therapeutically.
While not yet FDA-approved specifically for PTSD, this treatment is currently available through expanded access programs and represents a significant frontier in trauma-informed care.
Complex PTSD: Understanding the Need for Specialized Treatment
Complex PTSD (C-PTSD) develops in response to prolonged, repeated trauma, particularly when that trauma occurred in childhood or within inescapable relational contexts such as domestic violence or prolonged abuse. C-PTSD shares the core features of PTSD but additionally includes:
- Severe emotional dysregulation and affect instability
- Deeply damaged self-concept and chronic shame
- Profound disturbances in relational functioning and trust
- Dissociative symptoms including depersonalization and derealization
PTSD treatment for complex presentations typically requires longer treatment timelines, a stronger emphasis on stabilization and safety before trauma processing begins, and modalities that address relational trauma specifically, such as IFS, attachment-focused therapy, and schema therapy.
Complementary Approaches That Support PTSD Treatment
While specialized trauma therapy forms the core of effective PTSD treatment, several complementary approaches meaningfully support the healing process:
Mindfulness-Based Stress Reduction (MBSR)
MBSR training helps trauma survivors develop the capacity to observe distressing thoughts and sensations without being overwhelmed by them, a foundational skill for tolerating the emotional activation that trauma processing requires.
Yoga and Movement-Based Practices
Trauma-sensitive yoga has demonstrated effectiveness in reducing PTSD symptoms, particularly in survivors of sexual trauma and childhood abuse, by helping reconnect the survivor to their body in a safe, empowering context.
Peer Support and Group Therapy
Sharing experiences with others who understand trauma’s impact can powerfully reduce the isolation, shame, and self-blame that PTSD frequently generates. Group-based PTSD treatment provides both social connection and the corrective experience of being heard and validated.
Sleep Hygiene and Nervous System Regulation Practices
Given that sleep disturbances are one of PTSD’s most debilitating symptoms, targeted sleep hygiene strategies, breathing practices, and nervous system regulation techniques such as the 4-7-8 breathing method and progressive muscle relaxation provide meaningful symptom relief between therapy sessions.
How to Choose the Right PTSD Treatment for You
Selecting the most appropriate PTSD treatment approach depends on several important factors:
- Type and nature of your trauma (single incident vs. complex, relational trauma)
- Current symptom severity and functional impairment level
- Previous treatment history and what has or has not been helpful
- Personal preferences regarding the level of direct trauma engagement required
- Availability of qualified trauma specialists in your area or via telehealth
- Co-occurring conditions such as depression, anxiety disorders, substance use, or chronic pain
A qualified, trauma-informed therapist can conduct a comprehensive clinical assessment and collaboratively develop an individualized PTSD treatment plan tailored to your unique history, needs, and therapeutic goals.
When to Seek PTSD Treatment Immediately
If you are experiencing any of the following, reaching out for professional PTSD treatment support without delay is critically important:
- Active suicidal thoughts or self-harm behaviors
- Inability to maintain basic daily functioning
- Severe dissociative episodes that impair safety
- Substance use escalating as a means of managing PTSD symptoms
- Complete social isolation and withdrawal from all relationships
Help is available, and you do not have to navigate trauma alone. Reaching out to a trauma-informed mental health professional is an act of profound courage and self-compassion.
Final Thoughts
PTSD treatment has never been more sophisticated, accessible, or genuinely effective than it is today. From EMDR and TF-CBT to somatic approaches and emerging psychedelic-assisted therapies, the landscape of trauma healing offers real hope for every survivor, regardless of how long they have been living with the weight of their experiences.
Recovery from PTSD is not about forgetting what happened or pretending trauma did not leave its mark. It is about integrating your experiences so they no longer control your present, restoring your nervous system’s capacity for safety, and rebuilding a life of connection, purpose, and genuine wellbeing.
The most important step in your PTSD treatment journey is simply the decision to begin.
